In 2014, paediatric neurosurgeon Steven Schiff approached our research team with a challenge: build an easy-to-use, portable magnetic resonance imaging (MRI) system at a fraction of the cost of a conventional scanner. He needed it to image the brains of children in Uganda with hydrocephalus, a build-up of fluid in the brain.
Hydrocephalus is the most common reason for neurosurgery in children worldwide; there are almost 200,000 cases each year in sub-Saharan Africa alone. Surgeons operate to divert the fluid but procedures often fail and follow-up imaging is needed. Other forms of scanning and monitoring are impractical for this condition: ultrasound cannot penetrate the skulls of children over the age of two and X-rays carry a radiation risk. MRI fits the bill.
MRI is an indispensable part of clinical care, with more than 100 million scans performed worldwide annually, and around 50,000 machines in hospitals and clinics. However, people in low- and middle-income countries (LMICs) have limited access to this technology, despite constituting more than 70% of the world’s population. For example, on average there are 0.7 MRI scanners per million people in Africa, compared with 55 per million people in Japan, 40 in the United States and 35 in Germany. Most systems are in big cities, distant from rural populations. Of the scanners in Africa, 39% use obsolete hardware and software1.

One MRI for 4.7 million people: the battle to treat Syria’s quake survivors
MRI scanners are expensive — it costs several million US dollars to purchase, install, maintain and operate one machine. They require a superconducting magnet a couple of metres long, which weighs 5–10 tonnes, cooled by liquid helium and housed in a shielded room to reduce electromagnetic interference. The scanners need a powerful energy source and chilled water to cool other components. Highly trained technicians are essential. Software and hardware upgrades cost tens to hundreds of thousands of US dollars each year. All of this is beyond the reach of research, education and health-care settings in LMICs.
What these nations need instead, are completely redesigned MRI systems that can be easily set up and run in rural settings and secondary health facilities. Local physicians need to have confidence in using them to diagnose and treat common life-threatening conditions. Since our first conversation with Schiff (who is based at Yale School of Medicine in New Haven, Connecticut), our groups at the Leiden University Medical Center in the Netherlands and Mbarara University of Science and Technology in Uganda have collaborated with researchers in Paraguay, Spain, the United States and Germany to develop and promote affordable MRI systems in LMICs.
Here we outline progress and highlight five key challenges on which researchers should concentrate. We focus on Africa, the region with which we have most experience, but similar situations exist in South America and South Asia.
Improve low-field technologies
The principle behind MRI was published 50 years ago this week in Nature by Paul Lauterbur2, a chemist from the United States who shared the Nobel Prize in Physiology or Medicine in 2003 with Peter Mansfield, a British physicist, for this work. Conventional MRI machines use powerful superconducting magnets to polarize hydrogen nuclei in tissue. Pulses of radio waves interact with the polarized nuclei, generating a voltage in detectors placed around the patient. Algorithms convert these signals into images in which physicians can distinguish between tissues on the basis of characteristics such as water or protein content and stiffness.
A compact, portable MRI system cannot be built by simply shrinking down existing designs or replacing components with cheaper alternatives. But small machines can be optimized to monitor specific conditions such as hydrocephalus.

Scientists at the Mbarara University of Science and Technology in Uganda.Credit: Wouter Teeuwisse and Tom O’Reilly
To start, the superconducting magnet can be replaced with a small permanent magnet, which is typically made of neodymium boron iron or samarium cobalt alloys. Such magnets produce a much weaker field (0.05 to 0.1 Tesla) than conventional machines (1.5 or 3 Tesla), and hundreds to thousands of times less signal.
Electrical components must be redesigned to run on less power and off mains electricity or batteries. Image-processing algorithms and hardware must be able to correct for external noise, so that no shielding is needed. And the software must be easy to operate with minimal training.
Over the past ten years, two types of low-field MRI system have been developed by various groups. We have designed a version that consists of thousands of tiny magnets (a few centimetres or less across) configured to optimize the strength and uniformity of the magnetic field around the patient. The system, a barrel roughly 50 cm long and 50 cm in diameter, with an open inner bore 31 cm across, is relatively light (around 75 kilograms) and can be assembled in modules without specialist tools or equipment3. The system can be positioned at the head of a hospital bed and the patient slid into it. Our scanner can be wheeled through a hospital, loaded into a car and operated using open-source software.
The second design is simpler and consists of two discs that are a few centimetres thick and 60–95 cm in diameter. The discs are made of magnetic material joined by one or two iron yokes, placed above and below the patient’s head4. This system, however, requires specialized equipment to assemble, weighs several hundred kilograms and has to be moved on a motorized carriage.

Could Africa be the future for genomics research?
The US company Hyperfine in Guilford, Connecticut, has commercialized this latter design, which is currently used alongside typical MRI systems in intensive-care units and emergency departments, mainly in the United States. It has been tested on people with brain haemorrhages, strokes, multiple sclerosis and brain injuries5. The Bill & Melinda Gates Foundation plans to place more than 45 such systems throughout LMICs to help researchers understand and address the impacts of maternal and infant health, malnutrition and disease on infant brain development. Similar research platforms have been developed in China and Hong Kong.
Currently both systems are capable of imaging the brain with a resolution of around 2 millimetres in 10 minutes. By comparison, a conventional MRI scanner might resolve structures smaller than one millimetre in a few minutes. Although the low-field systems’ performance is sufficient for straightforward conditions such as hydrocephalus, it can be improved. Researchers must design more sensitive detectors, increase image contrast and deploy advanced image reconstruction methods, for example, using artificial intelligence (AI). They also need to ensure that systems operate reliably, robustly and reproducibly in challenging environmental conditions that are likely to be encountered, for example, in rural settings in LMICs.
Build physicians’ confidence
Conventional MRI is a specialist practice, usually handled by radiologists who are familiar with all the nuances. For uptake in LMICs, it’s crucial that physicians see low-field MRI technology as ‘smart-tech’ rather than ‘low-tech’, and not just a cheap alternative to the systems used in high-income countries (HICs).
Building this confidence requires clinicians and scientists to share their understanding of the information contained in the ‘grainier’ images obtained with low-field MRI. There’s currently little knowledge of, and few data on, how to use these devices clinically. MRI scientists need to ensure that the quality of low-field images is robust and reproducible and that, as with conventional scanners, any non-clinical artefacts are easy to spot. Simple user interfaces need to be designed and improved by working with clinicians and technicians in LMICs.
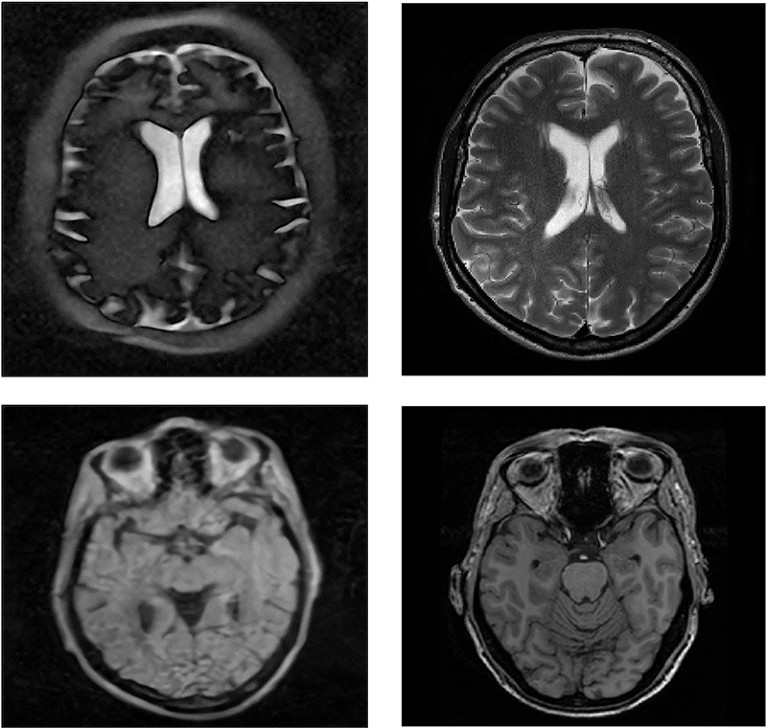
Scans from a low-field MRI system (left) compared with typical MRI scans.Credit: Leiden University Medical Center
Training programmes need to be developed for clinicians, including showing them how low-field images compare with conventional high-field and other types of scan. Acquisition of these images should be performed in both HICs and LMICs — in the former because of greater hardware availability and in the latter to ensure relevance to local health issues. The MRI community must make the case and prove that low-field images are clinically useful.
Prioritize open-source approaches
Commercial MRI scanners use proprietary software and hardware. This limits the extent to which medical physicists and engineers can understand and repair these systems. Many places do not have such expertise available locally. The World Health Organization (WHO) estimates that 70% of medical equipment donated to LMICs cannot be used because of insufficient training.
Scientists, clinicians and medical technologists in LMICs need to be empowered to design, maintain and build low-cost MRI systems on site6. And to do so, they need access to open-source hardware and software, in line with the United Nations’ 2020 Roadmap for Digital Cooperation, which stresses the need for digital inclusion for all, and for building architectures for digital cooperation.

Three ways to make proton therapy affordable
As an example, last year we designed a low-field MRI scanner ‘kit’ based on open-source hardware and software and shipped it from Leiden to our engineering college in Mbarara. Biomedical engineering students from six sub-Saharan African countries used the kit to construct the first portable, custom-built MRI system on-site in Africa, which is now being used to train students.
This project highlights the importance of funding, whether it’s from agency, governmental or corporate organizations, for encouraging open-source technology. Licences that allow technologies to be distributed widely while maintaining rights for developers are emerging, as are royalty-free sublicences that require a certain proportion of systems be sold at cost in LMICs. Such agreements are allowing some pharmaceutical companies to share COVID-19 vaccine technologies in Africa, for example.
What can researchers do? They can make data and code available in repositories, such as GitHub, and ensure that code is written in open-source languages. They can document methods and hardware developments on freely available websites (such as opensourceimaging.org). And they can help to adapt the academic culture, so that transparent and reproducible research is highly valued.
Develop AI tools for LMIC contexts
Using AI to detect simple abnormalities in medical images can improve outcomes and save costs in nations where training is hard to access. AI might also be helpful for ‘task-switching’, in which nurses and medical technicians take on roles typically filled by clinicians. However, most current AI applications, both commercial and research, are targeted to circumstances in HICs.
Efficient AI algorithms for low-field scanners in LMICs must be customized for specific equipment and trained on local images. Data from HICs might not be relevant to populations in LMICs, owing to different spectra of disease, genetics and environmental differences7. Local data privacy laws must be considered, because these vary by country8. Images from other types of scan (such as computed tomography) that are more widely used in LMICs can be incorporated into training data. Eventually, low-field MRI systems themselves could be instrumental in increasing the size and diversity of AI training data sets, because these devices can be taken into patients’ homes9.
Boost funding for sustainable MRI
Collectively, we found it hard to secure funding for our compact MRI system. Governments in the United States and Europe prioritize high-end instrumentation that directly benefits their residents. Research that simplifies instruments, particularly for use in LMICs, is seen as a lower priority. Philanthropic foundations are more amenable but have their own priorities and can be hard to access without the right contacts. In our case, we managed to use a small amount of initial funding from the Dutch Research Council (NWO) as a stepping stone to further grants from the European Union and US National Institutes of Health.
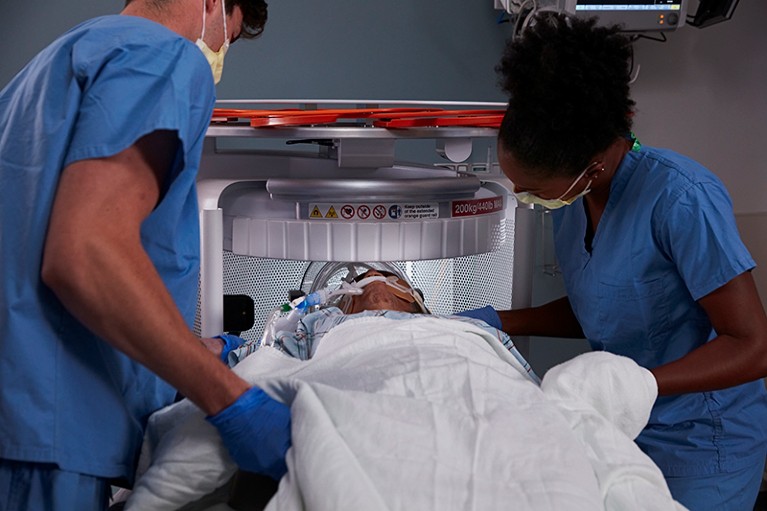
A patient is slid into a portable MRI system, which is produced by the US company Hyperfine.Credit: Hyperfine, Inc.
This funding gap might stem from a lack of awareness of medical needs in LMICs. Fewer than 1% of attendees at major MRI research and radiological meetings are from institutions in LMICs1. Similarly, research publications on MRI from LMICs make up less than 1% of global output, with the majority coming from collaborations with scientists in HICs1. A research brain drain from LMICs is well documented10. Yet, developing low-field MRI into a clinical tool rivals the hardest challenges in medical imaging today.
In HICs, medical-imaging research involves networks of companies, government-funded laboratories and university research and education programmes. Personnel and ideas flow between these entities, enabling sustained long-term collaborations. Similar networks need to be set up in LMICs, with early-career researchers at the heart to take these technologies forward.
There are encouraging signs of change. In 2019, the European Society for Magnetic Resonance in Medicine and Biology formed a network — the Consortium for Advancement of MRI Education and Research in Africa (CAMERA; see cameramriafrica.org). With more than 54 academic volunteers, 114 radiology residents and 54 medical physics trainees across 18 African countries, CAMERA organizes local events and supports researchers’ applications for funding. In 2022, the consortium assessed MRI use across sub-Saharan Africa, highlighting gaps in training, maintenance and research capacity1. Larger societies are beginning to mirror such efforts, including the International Society for Magnetic Resonance in Medicine (ISMRM) and various European and US radiology societies.
To ensure that LMIC scientists are involved, we advocate that financial obstacles to society membership and conference attendance be removed. Stop-gap measures, such as online-only access and associate memberships, are not enough, because they lack the benefits offered to full members, such as networking, building community awareness and the right to vote. Major organizations need to arrange their annual conferences in LMICs on a regular basis.
As Schiff’s challenge showed us, improving global health demands more than a piecemeal approach. Creative concepts from researchers and physicians can make MRI accessible to everyone.
link

